Emergency Medicine Physician Wellness in May: Burnout, Mental Health, and How to Protect Yourself
Mental Health Awareness Month in May is more than a calendar event for emergency medicine physicians. It is a necessary checkpoint. The reality is simple: the demands of emergency medicine continue to push physicians to their limits, and the data shows it clearly.
The State of Emergency Medicine Physician Mental Health
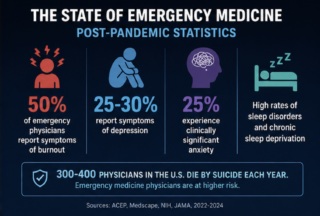
Emergency medicine physicians face some of the highest rates of burnout in healthcare. Recent post-pandemic data suggests that approximately 50% of emergency physicians report symptoms of burnout, driven by long shifts, high patient volume, administrative burden, and repeated exposure to trauma.
But burnout is just the surface.
- Depression: Around 25–30% of emergency physicians report symptoms of depression
- Anxiety: Roughly 25% experience clinically significant anxiety
- Sleep disorders: Shift work and circadian disruption contribute to chronic sleep deprivation and insomnia in a large percentage of physicians
These are not isolated issues. They compound over time and begin to affect physical health, cognitive performance, and patient care.
The Post-Pandemic Reality
The COVID-19 pandemic intensified existing stressors and introduced new ones: moral injury, resource scarcity, and prolonged uncertainty. While the acute phase has passed, the aftereffects remain.
Physician suicide continues to be a critical concern. Estimates suggest that 300–400 physicians in the United States die by suicide each year, with emergency medicine physicians considered a higher-risk group due to the nature of their work. Burnout rates have not returned to pre-pandemic baselines, and in many systems, they’ve worsened.
The Physical Toll of Burnout
Burnout is not just mental. It shows up physically in ways that are often ignored:
- Chronic fatigue and low energy
- Headaches and migraines
- Gastrointestinal issues
- Increased risk of hypertension and cardiovascular disease
- Weakened immune function
- Substance use as a coping mechanism
Over time, these symptoms can evolve into long-term health conditions if left unaddressed.
Why Emergency Medicine Is Uniquely Vulnerable
Emergency physicians operate in an environment defined by:
- Unpredictability and lack of control
- High-stakes, rapid decision-making
- Frequent exposure to trauma and death
- Irregular schedules that disrupt sleep and recovery
- Limited continuity of care, which can reduce a sense of closure or reward
This combination creates the perfect storm for emotional exhaustion and detachment if protective measures are not in place.
Practical Strategies to Protect Your Mental Health
There is no single fix, but there are proven ways to reduce risk and build resilience.
1. Protect Your Sleep Aggressively
Treat sleep as a non-negotiable. Use blackout curtains, limit caffeine late in shifts, and create consistent wind-down routines after nights.
2. Build a Real Support System
Peer support matters. Whether it is colleagues, mentors, or a therapist, having people who understand the job reduces isolation and normalizes the struggle.
3. Set Boundaries Where You Can
Emergency medicine limits control, but not entirely. Be intentional about scheduling preferences, time off, and saying no when possible.
4. Move Your Body Regularly
Exercise is one of the most effective ways to regulate stress, improve mood, and counteract the physical effects of burnout.
5. Limit Maladaptive Coping
Alcohol, isolation, and overwork can quietly become default coping mechanisms. Recognizing these patterns early is critical.
6. Use Professional Resources Without Hesitation
Employee assistance programs, confidential counseling, and physician support lines exist for a reason. Using them is not a weakness, it is maintenance.
7. Reconnect With Meaning Outside the ED
Hobbies, family, time outdoors, and non-medical interests provide psychological distance from the job and help restore perspective.
Changing the Culture
One of the biggest barriers to physician wellness is culture. Medicine has historically rewarded endurance over sustainability. That has to shift.
Talking openly about mental health, supporting colleagues who are struggling, and normalizing help-seeking behavior are not soft initiatives. They are necessary changes to preserve the workforce and improve patient care.
Final Thoughts
Emergency medicine physicians are trained to prioritize others in moments of crisis. But Mental Health Awareness Month is a reminder that ignoring your own well-being comes at a cost.
Taking care of yourself is not optional. It is part of doing the job well and staying in it long enough to matter.
If you are feeling the weight of burnout, anxiety, or depression, addressing it early is one of the most important clinical decisions you can make—just for yourself this time.


