GLP-1 Drugs Like Semaglutide: What the Science Actually Says (Without the Hype)
A few years ago, drugs like semaglutide were just another tool for managing Type 2 Diabetes. Now they’re being talked about like they might change everything from obesity to aging to addiction.
Whenever something gets that much attention that quickly, the signal gets buried under noise. Some of what you’re hearing is backed by strong clinical evidence. Some of it is early-stage science being stretched into conclusions it hasn’t earned yet.
If you strip away the marketing and the headlines, the real story is more grounded and, in some ways, more interesting.
Why These Drugs Work So Well in the First Place
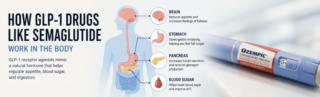
GLP-1 receptor agonists don’t do anything exotic. They amplify a system your body already uses to regulate food intake and blood sugar. After you eat, your body releases GLP-1 to help coordinate insulin release, slow digestion, and signal that you’ve had enough.
Semaglutide essentially strengthens that signal.
Food stays in the stomach longer, appetite drops, and blood sugar spikes are blunted. People don’t have to “try harder” to eat less. They just… do. That’s the piece most diets fail to solve, and it’s why these drugs have had such an outsized impact.
The Results in Diabetes and Obesity Are Not Subtle

In Type 2 Diabetes, the benefit is straightforward and well-established. Blood sugar improves, long-term complications are reduced, and large cardiovascular outcome trials have shown fewer heart attacks and strokes in high-risk patients. This isn’t emerging science. It’s already part of standard care.
Where things really shifted public attention is obesity.
In the STEP trials, people weren’t losing five pounds here and there. They were losing double-digit percentages of their body weight and, more importantly, keeping a meaningful portion of it off while on the medication. That changes risk profiles across the board, from blood pressure to lipid levels to systemic inflammation.
It’s one of the first times a medication has consistently produced that level of weight loss without surgery. That alone explains most of the excitement.
The Liver Story: Real Improvements, Overstated Conclusions
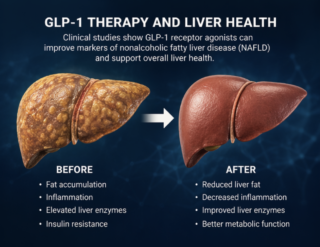
There’s also been a surge of interest in how these drugs affect Nonalcoholic Fatty Liver Disease, which is tightly linked to obesity and insulin resistance.
Clinical studies show that liver fat decreases, enzyme levels improve, and markers of inflammation trend in the right direction. For a condition that often progresses silently toward more serious disease, that matters.
But this is where language starts to drift.
You’ll see claims about “liver regeneration,” which implies something far more dramatic than what’s actually been demonstrated. The current evidence supports improvement in liver health, not the regrowth of damaged liver tissue in a true regenerative sense. A lot of the benefit appears to come from weight loss and better metabolic control, not a direct rebuilding of the liver itself.
That distinction gets lost in translation, especially outside medical literature.
Anti-Aging: Mechanistically Interesting, Clinically Unproven
The anti-aging conversation is even more prone to exaggeration.
At the cellular level, GLP-1 signaling appears to influence processes that are tightly connected to aging: oxidative stress, inflammation, mitochondrial efficiency, and even pathways related to cellular senescence. In animal models, those effects look promising.
But promising mechanisms are not the same as proven outcomes.
In humans, we do not have clinical trials showing that semaglutide slows aging or extends lifespan. What we do have is something more indirect: people on these medications often improve the exact risk factors that drive age-related disease in the first place. Cardiovascular disease risk drops. Metabolic health improves. Complications tied to obesity and diabetes become less likely.
That can absolutely translate into living longer or healthier lives. It just doesn’t mean the drug itself is an anti-aging therapy in the way people are starting to describe it.
The Unexpected Angle: Addiction and Alcohol Use
One of the more intriguing areas of research is how GLP-1 drugs affect behavior, particularly around reward.
Early studies, including animal models and small human observations, suggest these drugs may reduce the desire for alcohol and dampen reward-driven consumption patterns. That has obvious implications for conditions like Alcohol Use Disorder.
The mechanism makes sense. GLP-1 receptors are present in parts of the brain that regulate reward and motivation. If those signals are being modulated, it could change how reinforcing certain behaviors feel.
But this is still early. There isn’t enough clinical evidence to treat GLP-1 drugs as a standard therapy for addiction. It’s a signal worth paying attention to, not a conclusion.
The Tradeoffs Are Real
For all the upside, these medications are not neutral.
The most common issues are gastrointestinal. Nausea, vomiting, and general digestive discomfort show up early for a lot of people, especially as doses increase. Some adapt. Some don’t.
More serious risks exist, even if they’re less common. Pancreatitis has been reported. Gallbladder issues appear more frequently in some patients. There are also ongoing questions about long-term effects, including signals seen in animal studies related to thyroid tumors.
Then there’s the practical reality most people don’t factor in at the beginning: when the medication stops, the biology it was controlling tends to come back. Appetite returns. Weight regain is common. For many people, this becomes a long-term or indefinite therapy, not a short intervention.
So Where Does That Leave All the Hype?
GLP-1 drugs like semaglutide are one of the most meaningful advances in metabolic medicine in decades. That part is justified.
They work. Not marginally, but in ways that change real clinical outcomes.
At the same time, they’re being asked to carry claims the evidence doesn’t fully support yet. They are not proven anti-aging drugs. They do not regenerate organs in the way headlines suggest. They are not a standalone solution that replaces behavior, diet, or long-term strategy.
They’re a powerful tool. And like most powerful tools, they work best when they’re used for what they actually do—not what people wish they did.

